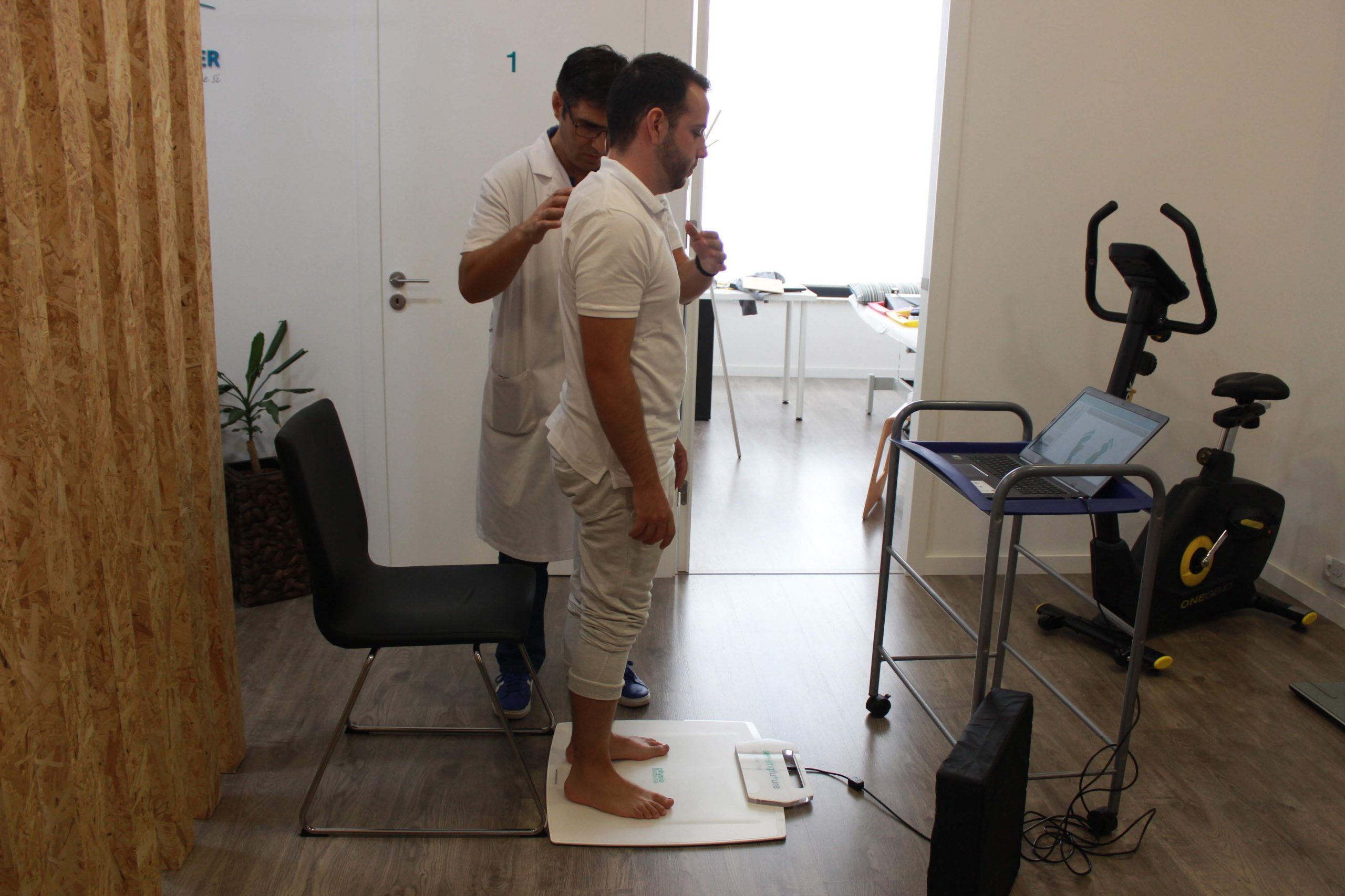
- A look at the Sit-to-Stand protocol
The Sit-to-Stand (STS) is a well-known test to quantify the ability of the patient to lift from a sitting position to a standing position. The STS maneuver is mainly used to assess lower limb strength, balance and also fall risk in elderly people [1].
There are several variations of the STS test, such as the five-repetition STS test (FRSTST) which report the amount of time it took to do the repetitions or the 30 second chair stand test (30CST) which involves counting the number of repetitions completed [2]. PhysioSensing Balance Software, using the presure plate, has a different version of the Sit-to-Stand, with three commanded repetitions, based on the research from Chang Gung Memorial Hospital and Chang Gung University [3].
- How is it done?
This protocol measures the STS performance on three 15-seconds trials:
- Lift from a sitting position to a standing position, as quickly as possible after indication in the interface (the words GET UP appear), without using the hands.
- Stand still until end of trial.
- Sit and repeat two more times.
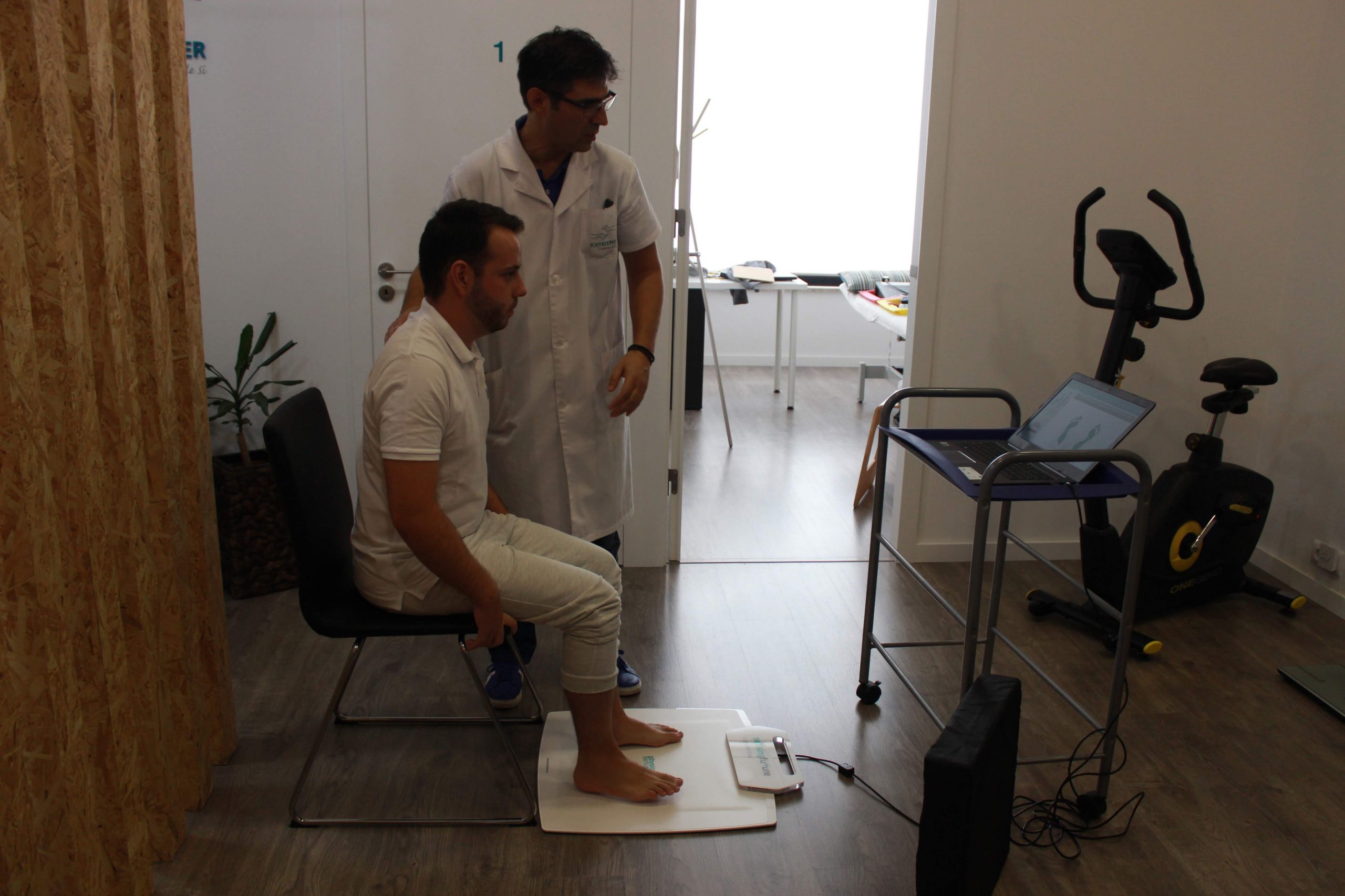 |
|
|
|
 | |
Figure 1 –Example and Interface of Sit-to-Stand protocol.
- Measures calculated
After performing the three trials of the protocol, the average values of the Weight Time Transfer, Rising Index, Sway Velocity and Left/Right Symmetry appear:
- The weight time transfer is the time between the indication to get up and the arrival of the center of pressure over the feet, i.e., the time required to transfer the weight from a seated position to the moment when all the weight is over the feet, in seconds.
- The rising index is the force exerted during the rising phase, from the lift off moment until the end of extension (start of standing position), expressed as a percentage of body weight.
- The sway velocity is the displacement of the center of pressure during the rising phase and the following 5 seconds (during stabilization phase), divided by the time (°/s).
- The left/right symmetry is the percentage of weight difference between the right and left leg during the rising phase and the following 5 seconds (during stabilization phase). The result bar points to the side that supports greater weight.
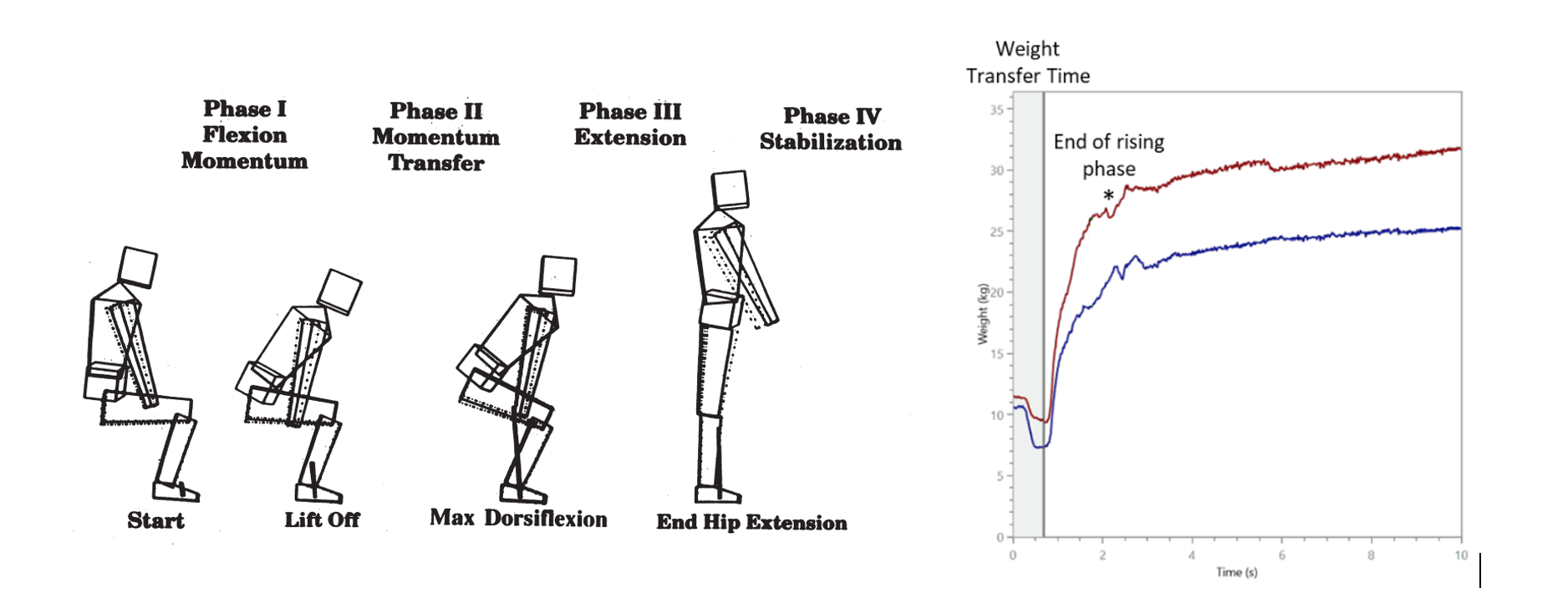
Figure 2 – (Left) Illustration of four phases of the sit-to-stand maneuver, from Frykberg, G. E., & Häger, C. K [2]. (Right) Weight values over time (for the left and right leg in blue and red, respectively), with indication of the weight transfer time in gray and the end of the rising phase with an asterisk, which corresponds to the end hip extension of the left image.
In addition, the center of pressure trace for each trial, as well as the weight variation over time, can be observed (Figure 3).

Figure 3 – Example of the results section for the STS protocol.
All this information can be quickly exported to a PDF report, and also view the progress between evaluations. This allows a more objective and quantitative look at the sit-to-stand movement.
- Significance
Lifting from a seated position to a standing position is influenced by several musculoskeletal, movement control, and balance factors. Results outside the normative values can be indicative of reduced range of motion and flexibility in the lower extremity or trunk (thus the weight time transfer can be slower), reduced trunk and lower limb strength or movement control impairments (which is mainly noted in low values of the rising index and higher values of sway velocity). These patients have difficulty in transitioning from a sitting to a standing position and may need assistance during the transition to avoid falls and injuries [3–5].
Healthy individuals use only their legs to exert the necessary force during the rising phase and then control the center of pressure over the base of support when reaching the standing position. The force during the rising phase is approximately symmetrical, for the right and left legs, for lateral stability.
As mentioned, the sit-to-stand is also a well-known preliminary screening tool for the risk of falling. There are several articles establishing the association between sit-to-stand performance and fallers patients [3], [6], [7]. According to Cheng, P.-T., et al. study, stroke fallers showed significantly lower rate of rise in force and higher postural sway while rising and sitting down [3]. In addition, Chou, S.-W., et al. has found significant correlation between sit-to-stand and gait parameters on hemiplegic patients. Hemiplegic stroke patients who took less time to rise and had a smaller difference of the maximal vertical force between both legs, had better gait performance [5].
It is also important to point out that instrumented assessment of sit-to-stand allows objective measurement, that is reproducible, practical, and reliable, allowing comparison and progress monitoring after rehabilitation.
You may also like read about 12 Protocols for Balance Assessment with force/pressure plate.
>>>> Check our solutions and ask now for a quotation
Cláudia Tonelo
Sensing Future Technologies
Bibliography
[1] R. W. Bohannon, D. J. Bubela, S. R. Magasi, Y.-C. Wang, and R. C. Gershon, “Sit-to-stand test: Performance and determinants across the age-span,” IES, vol. 18, no. 4, pp. 235–240, Nov. 2010, doi: 10.3233/IES-2010-0389.
[2] G. E. Frykberg and C. K. Häger, “Movement analysis of sit-to-stand – research informing clinical practice,” Physical Therapy Reviews, vol. 20, no. 3, pp. 156–167, Jun. 2015, doi: 10.1179/1743288X15Y.0000000005.
[3] P. T. Cheng, M. Y. Liaw, M. K. Wong, F. T. Tang, M. Y. Lee, and P. S. Lin, “The sit-to-stand movement in stroke patients and its correlation with falling,” Arch Phys Med Rehabil, vol. 79, no. 9, pp. 1043–1046, Sep. 1998, doi: 10.1016/s0003-9993(98)90168-x.
[4] S. B. O’Sullivan and T. J. Schmitz, Physical rehabilitation (5th Ed.). FA Davis, 2007.
[5] S.-W. Chou, A. M. K. Wong, C.-P. Leong, W.-S. Hong, F.-T. Tang, and T.-H. Lin, “Postural Control During Sit-to Stand and Gait in Stroke Patients,” American Journal of Physical Medicine & Rehabilitation, vol. 82, no. 1, pp. 42–47, Jan. 2003, doi: 10.1097/00002060-200301000-00007.
[6] S. Buatois et al., “Five Times Sit To Stand Test is a Predictor of Recurrent Falls in Healthy Community-Living Subjects Aged 65 and Older,” Journal of the American Geriatrics Society, vol. 56, no. 8, pp. 1575–1577, Aug. 2008, doi: 10.1111/j.1532-5415.2008.01777.x.
[7] A. Tiedemann, H. Shimada, C. Sherrington, S. Murray, and S. Lord, “The comparative ability of eight functional mobility tests for predicting falls in community-dwelling older people,” Age and Ageing, vol. 37, no. 4, pp. 430–435, Jul. 2008, doi: 10.1093/ageing/afn100.